《工作細胞》是部難得的微科學漫畫,敘述帥氣的白血球先生,與呆萌紅血球小姐的冒險故事。儘管裡頭充滿了努力、友情、正義必勝的故事,白血球們總是能夠一次又一次殺爆入侵的微生物(其實我比較想看微生物贏 XD)。但,真實的世界又是如何呢?

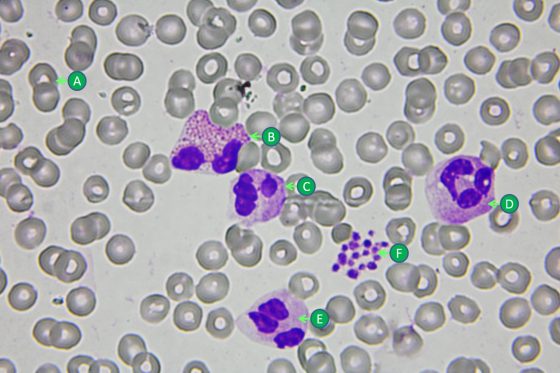
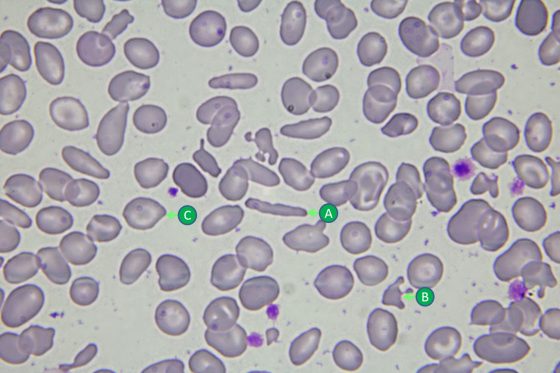
紅血球其實像顆貝果麵包,至於白血球咩,比較像是顆煎壞的荷包蛋……
《工作細胞》裡的角色多是可愛的紅血球小姐、帥氣的白血球先生,和萌萌的血小板蘿莉。但在真實的世界裡,它們的長相可就不是如此了,紅血球通常直徑為6~8 μm,長的很像一顆扎實的貝果麵包;而白血球稍大,直徑為9~12 μm,長的很像……一顆沒煎好的荷包蛋(我實在想不到其他的形容詞啊啊啊!)。
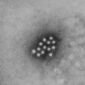
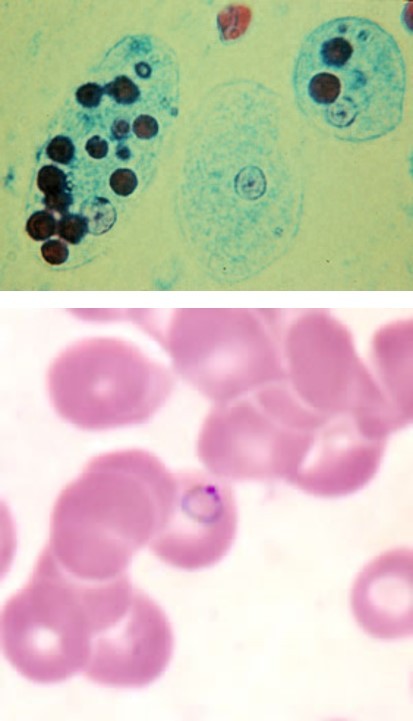
對細菌、病毒和寄生蟲而言,人體是個溫暖又不乏食物的地方,所以倘若有機會,這些求生存的浪浪微生物就會進入我們溫暖的肉體裡,與免疫細胞們共同上演一場又一場的生存之戰。大型的入侵者,如阿米巴原蟲,會吞食紅血球作為食物;小的如瘧原蟲會鑽入紅血球體內,不但能直接吸取營養,更可躲避白血球的攻擊 [1];而更高招的是那群反轉錄病毒(如:肝炎病毒Hepatitis Virus,和引起愛滋病的人體免疫缺陷病毒Human Immunodeficiency Virus/HIV),把自己的遺傳密碼直接寫入宿主細胞的DNA裡,不僅無需擔心白血球的攻擊,更潛藏於身體裡的細胞,幾乎無法根除,成了人體的一部份 [註1]!
對細菌來說,白血球才是可怕的惡魔!
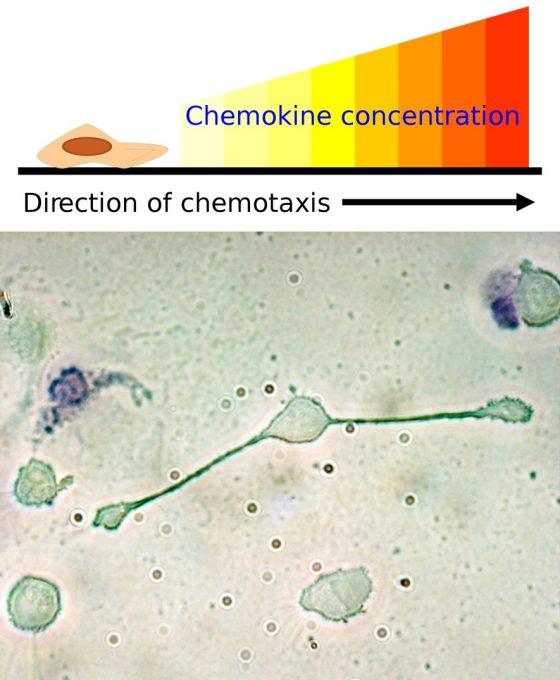
在這裡我要先替細菌說說話,其實以一隻小細菌的觀點來說,白血球超可怕的啦!彷彿就是《進擊的巨人》裡的食人巨獸般 [註2],利用靈敏的受器「聞」到發炎物質後,會成群結隊的奔襲而來(化學趨向性/Chemotaxis)。

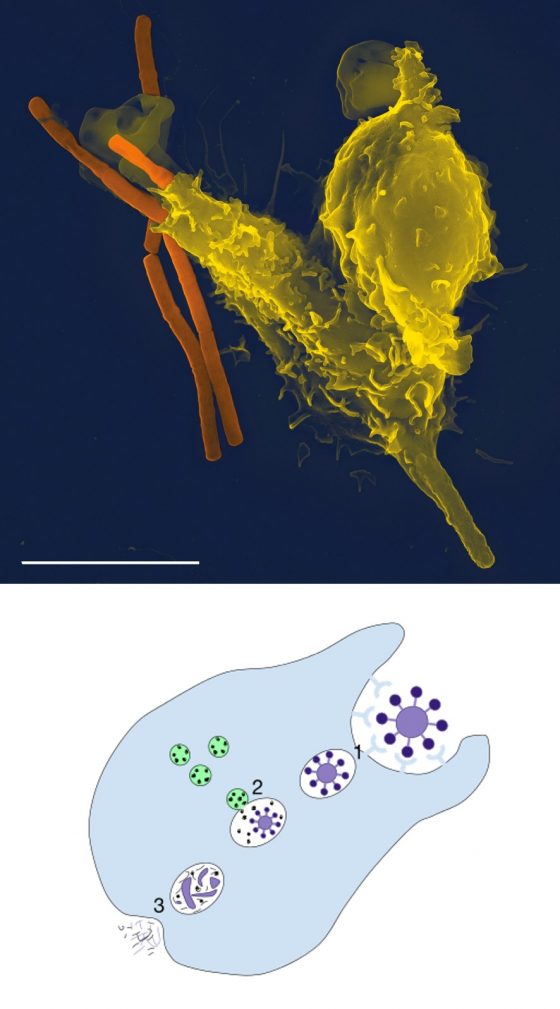
更可怕的是,一旦發現無助的細菌們,白血球會伸出巨大的偽足(pseudopodia)加以捕捉、吞噬。可憐的細菌被巨大的白血球吞食之後,還會被白血球體內的過氧化物、酵素等分解成碎片,一命嗚呼~而且被撕成碎片的屍體還會被巨噬細胞剪成胜肽(peptide)片段,送給免疫系統的老大-T細胞(T-helping cell)進一步刺激免疫反應,以召喚更多的白血球來襲擊細菌村莊 [3]!想想,以細菌的角度來看,白血球完全不是帥氣的型男衛兵,根本就是《沉默的羔羊》裡的變態食人魔吧 [註3]!
漫畫太善良了!真實的世界充滿陰謀詭計!
在《工作細胞》的前幾話中,出現的敵人都是少量的細菌,白血球們經過一番苦戰之後,總是會獲得最後的勝利。就算是腫瘤細胞也是僅用兩話的時間就清除得乾乾淨淨!但免疫系統遠比科學家們想像的還要複雜、神奇許多,真實的細胞世界裡充滿了計謀、背叛和策反之計!
比方說在人類歷史上佔有一席之地的結核桿菌(就是那隻能讓人得到肺結核、咳到吐血的原兇),是少數能夠潛藏在巨噬細胞的細菌,最近更被發現會利用巨噬細胞的訊息傳遞來提高自己的致病力 [4]!而近年來科學家更發現,腫瘤組織會吸引巨噬細胞聚集,讓它們釋放生長因子,進一步地刺激腫瘤細胞生長、茁壯 [5]!如此神奇、工於心計的免疫世界,未來是否也會在《工作細胞》裡出現呢?這是多麼的令人期待啊!(台灣的教育部快把《工作細胞》列為必讀書刊吧!)
- 註1:有一種理論是,遠古的反轉錄病毒將它們的基因寫入人體細胞後,經過很久很久的時間後,兩方達成了和平共存的狀態,也就逐漸變成了我們基因的一部份。
- 註2:《進擊的巨人》是近期風靡日本、台灣的漫畫,設定是類似於中世紀文明的世界裡,出現了喜食人類的巨人,引起了人類社會中難以想像的恐慌。
- 註3:《沉默的羔羊》為1991年上映的驚悚電影,男主角為冷酷的食人魔罪犯-漢尼拔醫師,其冷靜、工於心計又殘忍血腥的形象讓人不寒而慄。儘管只有21分鐘的戲份,其精湛的演技讓演員安東尼·霍普金斯成為奧斯卡獎史上,演出時間最短的男主角的獲獎演員。
本文感謝衛生福利部台東醫院檢驗科張昱維(Yu-Wei Chang)協助。
參考文獻
- 瘧疾(Malaria)。中華民國衛生福利部疾病管制署
- Galani IE, Andreakos E. Neutrophils in viral infections: Current concepts and caveats. Journal of Leukocyte Biology, 2015, 98, 557-564
- 林建中、陳光偉、陳證文、王世輝。免疫樹突狀細胞之簡介。中華民國醫師公會全國聯合會
- 結核桿菌的一個新發現的致病機制。Nature期刊
- Elaine Y. Lin, Jiu-Feng Li, Leoid Gnatovskiy, Yan Deng, Liyin Zhu, Dustin A. Grzesik, Hong Qian, Xiao-nan Xue, Jeffrey W. Pollard. Macrophages Regulate the Angiogenic Switch in a Mouse Model of Breast Cancer. Cancer Research. 2006. DOI: 10.1158/0008-5472.CAN-06-1278
___________
你是國中生或家有國中生或正在教國中生?
科學生跟著課程進度每週更新科學文章並搭配測驗。來科學生陪你一起唸科學!